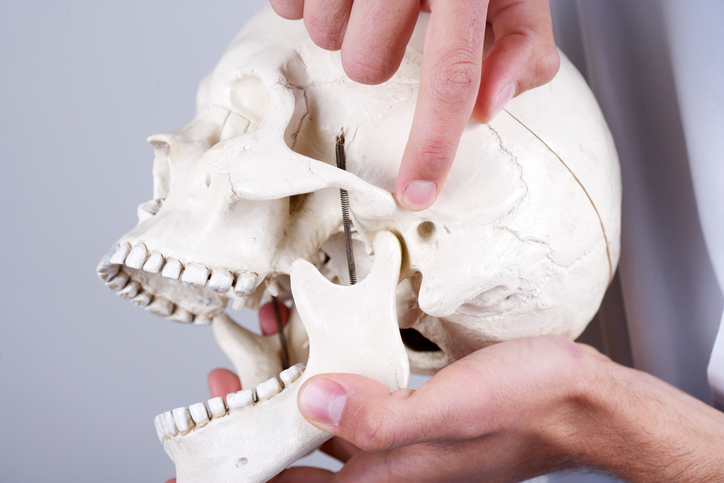
The temporomandibular articulation is composed of a group of anatomical structures including the bilateral, diarthrodial, and temporomandibular joints (TMJs). The TMJ and its associated structures play a key role in mandibular motion and redistributing stress from daily tasks such as chewing, swallowing, and speaking. TMJ disorders, or TMD, refer to a group of conditions that cause pain and dysfunction in the jaw joint and the muscles controlling the jaw.1 As a degenerative musculoskeletal condition, TMD is associated with morphological and functional deformities including abnormalities in the intra-articular discal position and dysfunction of the surrounding musculature.2 Common symptoms include painful joint sounds, restricted range of motion, and orofacial pain.
Although signs of TMD appear in 60-70% of the general population, only one in four individuals actually report symptoms.3 The frequency of severe symptoms (e.g. headaches and facial pain) associated with an urgent need of treatment is 1-2% in children, 5% in adolescents, and 5-12% in adults.4 Furthermore, studies in the 1980s found TMD symptoms in 16-59% of the general population, with only 3-7% of the adult population seeking treatment. A major risk factor for TMD is gender as symptoms appear four times as often in females than in males. Females also represent the vast majority of the patient population, with nearly 90% of TMD patients being female.4
Nearly 70% of TMD patients suffer from internal derangement, which refers to a malpositioning of the TMJ disc. Although the progression of TMD is not fully understood, the present evidence points to osteoarthritis (for inflammatory states) and osteoarthrosis (for non-inflammatory states) as the primary pathologies.5 For example, Bertram et al found that 54.2% of patients with unilateral TMD suffered from osteoarthritis in the affected joint.6 In contrast to asymptomatic patients, who show minimal morphological change in the condyle and articular eminence, symptomatic patients with internal derangement show substantial osseous change over time. Osteoarthritic changes associated with TMD may include deterioration of the articular cartilage and thickening of the underlying bone.1 Once joint breakdown begins, osteoarthritis can become crippling and eventually lead to significant morphological deformity and functional obstruction.
Treatment options for TMD vary with respect to the severity of degeneration. Non-invasive modalities include physical therapy, occlusal splints, and pharmacologics. Physical therapy for TMD involves electrophysical modalities (e.g. transcutaneous electric nerve stimulation) and manual techniques aimed at relieving pain in the joint and improving range of motion.7 Physical therapists may also implement behavior changes by altering the patient’s posture, diet, and stress-related habits. In previous studies, manual therapies demonstrated promise in treating TMD, especially when combined with exercise regimens aimed at strengthening the masticatory and cervical spine muscles to enhance mobility.8 Pharmacologic agents commonly prescribed to TMD patients include non-steroidal anti-inflammatory drugs (NSAIDs) and muscle relaxants. Minimally invasive therapies for TMD include sodium hyaluronate and corticosteroid injections, arthrocentesis, and arthroscopy.1 In the 5% of cases where nonsurgical methods fail, open joint surgery is potentially necessary to restore mandibular motion and relieve orofacial pain. Open joint surgery commonly involves discectomy, reshaping the articulating surfaces, and implanting alloplastic materials.9 When the negative effects of joint degeneration and pain exceed the potential benefit of less invasive surgical methods, total joint replacement may be required.
References
- Zarb GA, Carlsson GE. Temporomandibular disorders: osteoarthritis. J Orofac Pain. 1999;13:295–306.
- Laskin DM, Greenfield W, Gale E. The President’s Conference on the Examination, Diagnosis, and Management of Temporomandibular Disorders. Chicago: American Dental Association; 1983.
- Graber, Rakosi, Petrovic . In: Dentofacial Orthopedics with Functional Appliances. 2nd ed. St. Louis: Mosby; 2009. Functional analysis- examination of temporomandibular joint and condylar movement; pp. 135–40.
- Athanasiou AE. Orthodontics and craniomandibular disorders. In: Samire, Bishara, editors. Textbook of orthodontics. 2nd ed. Philadelphia: Saunders; 2003. pp. 478–93.
- Farrar WB, McCarty WL., Jr The TMJ dilemma. J Ala Dent Assoc. 1979;63:19–26.
- Bertram S, Rudisch A, Innerhofer K, Pumpel E, Grubwieser G, Emshoff R. Diagnosing TMJ internal derangement and osteoarthritis with magnetic resonance imaging. J Am Dent Assoc. 2001;132:753–61.
- McNeely ML, Armijo Olivo S, Magee DJ. A systematic review of the effectiveness of physical therapy interventions for temporomandibular disorders. Phys Ther. 2006;86:710–25.
- Rocabado M. The importance of soft tissue mechanics in stability and instability of the cervical spine: a functional diagnosis for treatment planning. Cranio. 1987;5:130–8.
- Dolwick MF. The role of temporomandibular joint surgery in the treatment of patients with internal derangement. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997;83:150–5.